Unless you have cancer, it is unlikely that you need a hysterectomy.
– Dr. Stanley West
The medical establishment has historically seen the uterus as expendable, despite the strong feelings
of many women to the contrary.
– Dr. Stanley West
Learn More
Dr. Stanley West is the author of The Hysterectomy Hoax, published in January, 1994 by Doubleday. In it he explains why 90 percent of all hysterectomies are unnecessary, and describes all the treatment options available to every woman, no matter what age.
Questions?
Contact Dr. West. He will answer you promptly


[Dr. West] told me he would absolutely not do a hysterectomy, and that there was no need for one.
–S. Bachner, New York
Dr. West restored my faith in physicians…[he] stated over and over again that…he would not perform a hysterectomy…I am forever in [his] debt.
– Kelli Greene,
Old Bridge, NJ.
I want to have children someday. My life would be over if I agreed to a hysterectomy.
Hysterectomy
Only ten percent of all hysterectomies are done for cancer. Because of this, Dr. West is certain that ninety percent of all hysterectomies are unnecessary. Unless you have cancer, it is unlikely that you need a hysterectomy. And it is prudent to be very sure that you DO have cancer before signing consent for the surgery.
Sixty percent of all hysterectomies in the U.S. are done in response to fibroids. Fibroids, by their very definition, are NOT cancer. The primary reason that so many hysterectomies are done instead of myomectomies (surgical removal of fibroids) is that medical schools spend a lot of time teaching hysterectomy and very little teaching myomectomy.
There are several reasons for this bias. Hysterectomy is simpler to perform and does not require as much training for the doctor. In addition, the medical establishment has historically seen the uterus as expendable, despite the strong feelings of many women to the contrary. Serious side effects that can develop as a result of hysterectomy have, until recently, been ignored by medical science.
Potential Side Effects
of Hysterectomy
Today it is well documented in the medical literature that many women develop serious health problems after hysterectomy. Depression; fatigue; urinary disorders; joint aches and pains; and unwelcome changes in sexual desire and response, including lack of libido and orgasm; are the most common complaints. These symptoms are real, and many of them have a medical explanation.
If a hysterectomy will save your life, the possibility of side effects such as these may be a necessary price to pay. And there is hope, because not all women experience these side effects. But in the case of fibroids, there is no reason to sacrifice the uterus and risk trading in one set of problems for another. Myomectomy in the hands of an expert is less radical surgery and does not pose the risk of these side effects.
Myomectomy vs. Hysterectomy
Myomectomy is the preferred choice for women wishing to have children and for those who simply wish to keep that option open. Many women, even those past their child-bearing years, do not see their uterus and ovaries as expendable organs. They do not wish to risk bringing on menopause the side effects of hysterectomy, especially when other options are available to them.
If before your myomectomy procedure your doctor asks you to consent to hysterectomy “just in case”, it is time to ask questions. If you sign a consent for hysterectomy “just in case”, then whether you wake up with a hysterectomy or myomectomy will depend on the skill level and preferences of this particular surgeon, not on your preference.
Questions to Ask Your Doctor about Hysterectomy
- How many myomectomies do you do? How many hysterectomies?
- How many women who go in for a myomectomy receive a hysterectomy instead?
- Have you ever completed a myomectomy on a woman with fibroids similar to mine?
- In my case, what circumstances would prevent you from following through on myomectomy and doing a hysterectomy instead?
Some doctors may get defensive. Because they have not had the appropriate training in myomectomy, they may tell you that myomectomies in many cases are dangerous or impossible. In reality, what they are telling you is that they do not have the expertise.
What is Hysterectomy?
Strictly speaking, hysterectomy means removal of the uterus. Not the ovaries and fallopian tubes. Just the uterus. When the ovaries and tubes also are removed in the course of surgery, the procedure is properly described as a hysterectomy and bilateral salpingo-oopherectomy.
The Three Approaches
To Hysterectomy
- Abdominal Hysterectomy
- Vaginal Hysterectomy
- Laparoscopic-assisted Vaginal Hysterectomy
Abdominal Hysterectomy
Abdominal hysterectomy is the most common surgical approach to hysterectomy, and is done through an incision in the abdomen. The main reason why hysterectomy is such simple surgery is that, internally, all women are built the same way. In every woman’s body the uterus is supported by the same ligaments and served by the same blood supply. Hysterectomy involves detaching the uterus from the ligaments that support it and the blood vessels that supply it.
COMPLICATIONS: If surgeons do their jobs carefully and meticulously, few women should suffer complications from surgery. But there are several pitfalls. These include “adhesions”, which is bleeding that can cause organs to attach to each other; injury to the bowel, bladder, and ureter; postoperative bleeding, and problems with wound healing.
Vaginal Hysterectomy
About 20 percent of all hysterectomies are vaginal procedures. Instead of opening the abdomen, the surgeon approaches the uterus through the vagina, detaches it, and pulls it out. Vaginal hysterectomy usually is reserved for women with uterine prolapse – a uterus that has lost its muscular supports and began to sag.
COMPLICATIONS: Although vaginal hysterectomies are generally regarded as less dangerous than abdominal hysterectomies, they present their own set of risks and complications, including fever and infection, bladder injury, and adhesions.
Laparoscopic-Assisted
Vaginal Hysterectomy
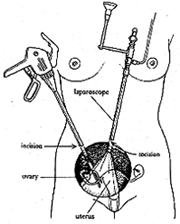 This new approach to hysterectomy involves the use of a viewing device called a laparoscope. The illustration shows how the laparoscope is inserted via a tiny abdominal incision near the belly button. Other surgical instruments are inserted through similarly small incisions. The big advantage of laparoscopic surgery of any type is that a small incision means a shorter hospital stay – only one or two days – less pain, and more rapid recuperation.
This new approach to hysterectomy involves the use of a viewing device called a laparoscope. The illustration shows how the laparoscope is inserted via a tiny abdominal incision near the belly button. Other surgical instruments are inserted through similarly small incisions. The big advantage of laparoscopic surgery of any type is that a small incision means a shorter hospital stay – only one or two days – less pain, and more rapid recuperation.
Because laparoscopic surgery involves so much less physical strain than conventional surgery, it has become very popular. Unfortunately, however, not all surgeons are as proficient as they should be before attempting the procedure. Some are operating on patients with no more training than merely having watched a film on laparoscopic surgery. This is a scary situation.
COMPLICATIONS: While laparoscopic-assisted vaginal hysterectomy is so new that we have no meaningful statistics on the rate of complications, there is no reason to believe that the complications would be any different from those that occur with other types of hysterectomy.The greatest threat is posed by inexperienced physicians who attempt the procedure without adequate training. The concern is that the availability of the procedure will lead to an increased number of unnecessary or unjustified hysterectomies.